My 5 month old daughter has what?!?!?
Infant Botulism, the nurse said. My wife and I both stood there dazed in the Pediatric Intensive Care Unit (PICU) at the Children’s Hospital of Philadelphia (CHOP). How could this be? She was laughing and giggling just 48 hours before. She never had a fever, a cough, sniffles, or any other sign that she was sick. She was just acting tired with a kind of weak moaning. When we called her doctors’ office we were told to just keep watching her temperature and make sure she was hydrated. In fact, if not for my wife’s insistence that “something is not right” we wouldn’t have even brought her to the emergency room.
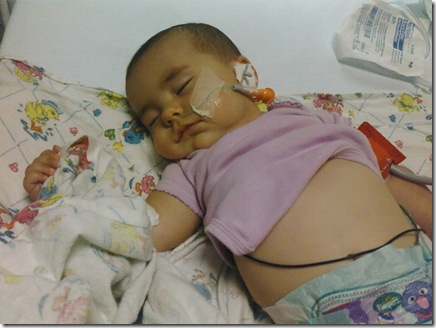 After Ava got to the hospital she was very listless and would not open her eyes. Even after a full day of being on a food tube with both breastmilk, pedialyte and saline she was not responding.
After Ava got to the hospital she was very listless and would not open her eyes. Even after a full day of being on a food tube with both breastmilk, pedialyte and saline she was not responding.
Rather then wait anymore time the doctors decided to get to action at once. The first thing she did was a spinal tap to see if it was spinal meningitis. Ava didn’t respond at all during the actual procedure which was cause for alarm. Babies usually cry or move in some way. The doctor then brought up the idea of Infant Botulism. She told us that we were going to be admitted to CHOP right away and a helicopter would take her into Philadelphia.
A helicopter we thought?? Wow – this is a lot more serious than we thought. Unfortunately, due to bad weather they could not fly her in and so my wife road with her in the ambulance and I followed not long after in the minivan. Our four year old daughter, Lauren, was told she would get to go “on vacation” with her grandparents for a few days while Mommy and Daddy took care of her sister. Little did we know it would be over a week before we would get to see Lauren again.
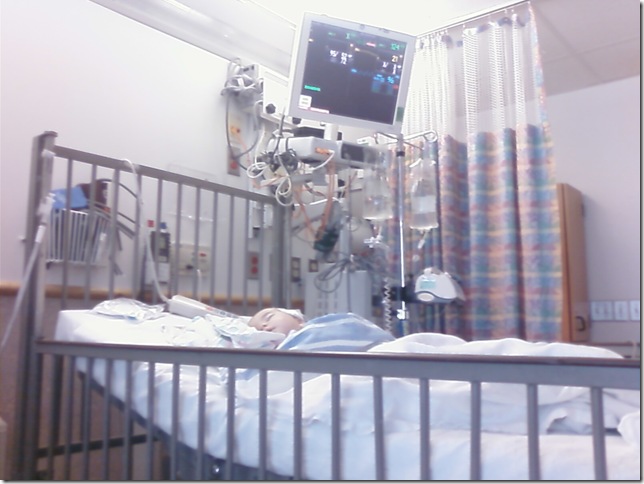
So there we stood with Ava in the PICU over Fourth of July weekend. Praying, hoping, and worrying. Knowing that she was in the best place possible for her right now but feeling helpless as parents.
We soon learned more about Infant Botulism and what it does. Basically there are bacterial spores that live in the air around us all time. As adults we have antibodies in our intestines that can fight them off. But infants under a year of age do not. The spores had gotten into Ava’s intestines and were releasing a nuerotoxin that affected the ability of the nerve endings in her muscles to respond to her brain. This created a paralysis and if not stopped it would eventually affect her diaphragm and she would not be able to breath on her own. But there was good news too. Ava had gotten medical treatment at the very early onset. She was still breathing on her own and even though her eyes were closed she was still conscious and would hold our hand if we gave it to her. There was also a drug, called BabyBIG, that could slow down the nuerotoxins and neutralize the spores within her. But the drug was only available in California and would need to be flown out to Pennsylvania.
It would take almost 24 hours for it to get to us. These were the hardest hours of our life. Ava’s NIF (negative inspiratory force) tests became borderline low and if she did not get the BabyBIG within a few hours she would need to go on a respirator. The nurses had the machine next to her bed all ready to go so there was no delay.
It was 6pm on Sunday when the BabyBIG finally arrived into the room. The miracle drug from California was here! They administered it through an IV and it was fully into her system in a few hours. She fell asleep after that and slept sound for almost a day. Then the miracle happened. She opened one eye a bit and smiled at daddy. I burst into tears and immediately called out for my wife. Within 24 hours she was doing things everyone told us may take weeks to come back. She moved her little feet up to her mouth, she was rolling on her side, she was focusing on stuff all over her room (especially the balloons my team had sent me!) and she was biting down on her toys. What a wonder baby!
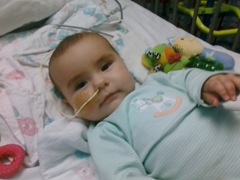
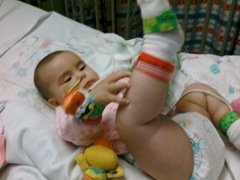
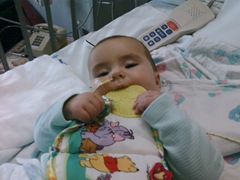
At this point the only thing other than the BabyBIG she was getting was my wife’s breastmilk. I am still amazed by Ava’s mom. She never once left the hospital and pumped breastmilk literally every hour to keep up with the food tube demands. The nurses were calling it “liquid gold” and it helped nurse her back faster than anyone had ever seen. Thank you so much Cheryl – I love you!
The last thing we were told that would come back was Ava’s ability to suck. But by the next day there she was breastfeeding! We could not believe it. First a little less than an ounce, then 2 oz, and then 3 oz. She was the little engine that could! She was back to her old self – smiling, laughing, playing. Our hearts were filled with Joy. Lauren was back from her grandparents and the next week I would spend bringing her to the hospital everyday to be with her sister and mom. The bond between my two girls, even at this age, is a strong one and Ava would light up every time her sister would come into the room. Lauren even took to reading her own made up stories to Ava.
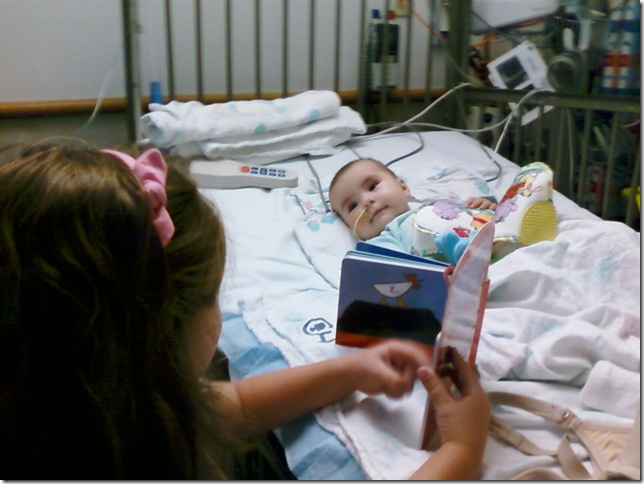
After over two and half weeks in the hospital Ava is now doing great and is back home with us. We are just monitoring her weight (it has been a bit down) to make sure she is getting enough calories to be back on track. She amazed the doctors with her progress. Stays in the hospital of up to 5 weeks are not unheard of with Infant Botulism so the fact that she is home already is a small type of miracle.

As far as how it happened, she never had honey (still exclusively breastfed) and the fact that we are not near new construction means she must have inhaled the spores somewhere. Evidently they are all over the place in southeast Pennsylvania (who knew?) and the incubation period is up to 30 days so it is almost impossible to know where she got it. The good news though is the anti-toxin they gave her (BabyBIG) will keep her immune for the next 6 months until her own body can fight it off.
It was a terrifying experience but we felt the circle of love close in around us from everyone Faith, Family, Friends – these bonds are all now stronger than ever.
I want to thank the doctors for diagnosing her so fast. The fact that she was treated early enough and never had any respiratory complications means she will most likely fully recover. But not all infants are so lucky. The bacteria spores exist everywhere and can be found in high concentrations in areas such as Califronia, Ohio and southeastern Pennsylvania. The only known method of prevention is to not give any infant under a year of age honey (of which most cases reported the infant never had honey) and to watch for early warning signs. If your child seems extremely listless, refuses to eat, and has a very weak cry take them to the emergency room immediately! Time is of the essence. I recorded a video during our stay that shows the listlessness and you can hear the weak cry. Hopefully it may help doctors in diagnosing the early warning signs as they were able to do with Ava.
To learn more how you can save a child’s life please check out the Children's Hospital of Philadelphia donation site.
Thank you, and may God bless!
- Dave
